Haemorrhoids
Introduction
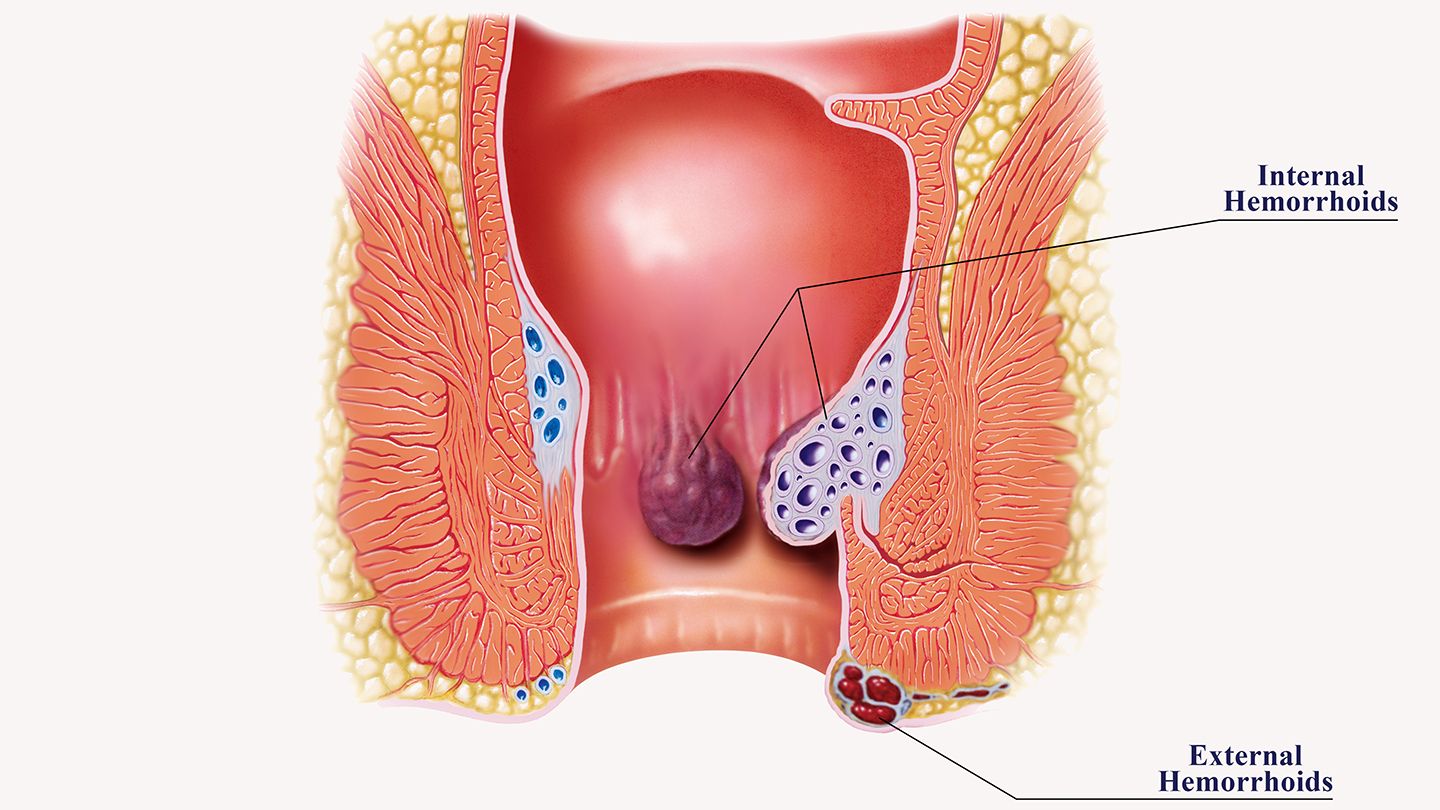
| Hemorrhoids, commonly referred to as piles, are vascular structures in the anal canal that play a crucial role in controlling bowel movements. While everyone has hemorrhoids, they become problematic when they undergo inflammation or swelling. There are two main types: internal hemorrhoids, which form inside the rectum and are often painless but may cause bleeding, and external hemorrhoids, which develop under the skin around the anus and can be more uncomfortable due to their proximity to nerve endings. The development of hemorrhoids is often associated with increased pressure on the pelvic and rectal veins, commonly occurring during straining during bowel movements, chronic constipation, or prolonged sitting. Pregnancy and obesity can also contribute to the development of hemorrhoids due to increased pressure on the pelvic region. As these veins become swollen, they can cause symptoms such as itching, pain, and bleeding, leading individuals to seek diagnosis and treatment for relief. |
 |
Medical History and Physical Examination:
- The first step in diagnosing hemorrhoids involves a thorough medical history and physical examination by a healthcare professional. Discussing symptoms such as pain, itching, and bleeding is crucial for an accurate diagnosis. A visual examination of the anal area is typically conducted to identify the presence of hemorrhoids.
- Proctoscopy or Anoscopy: For a more detailed examination, a proctoscopy or anoscopy may be performed. These procedures involve the use of a slender tube with a light and camera to inspect the rectum and anal canal, allowing the healthcare provider to visualize internal hemorrhoids.
- Colonoscopy: In some cases, a colonoscopy may be recommended to rule out other potential causes of symptoms and to ensure there are no complications or underlying issues in the colon.
Treatment Options
Lifestyle Modifications:
Mild cases of hemorrhoids can often be managed with lifestyle changes. These may include maintaining a high-fiber diet, staying hydrated, and avoiding prolonged periods of sitting or straining during bowel movements.
Topical Treatments:
Over-the-counter creams, ointments, and suppositories containing ingredients like witch hazel or hydrocortisone can help alleviate symptoms such as itching and inflammation. However, these are typically more effective for external hemorrhoids.
Sitz Baths:
Soaking the anal area in warm water, known as a sitz bath, can provide relief from pain and discomfort associated with hemorrhoids. This can be done several times a day for optimal results.
Rubber Band Ligation:
For internal hemorrhoids, a common treatment is rubber band ligation. This procedure involves placing a small rubber band around the base of the hemorrhoid, cutting off its blood supply. The hemorrhoid eventually shrinks and falls off.
Hemorrhoidectomy:
In severe cases or when other treatments fail, a surgical procedure called hemorrhoidectomy may be recommended. This involves the surgical removal of the hemorrhoids.




